Deep Brain Stimulation in Thane for Parkinson's Disease, Tremor, and Movement Disorders
If Parkinson’s symptoms are no longer staying well controlled with medicines, or tremor and movement problems are beginning to affect daily life despite treatment, Deep Brain Stimulation in Thane may be considered after a careful specialist evaluation.
DBS is an advanced treatment option used for selected patients with Parkinson’s disease, essential tremor, and some forms of dystonia. It is not the first step. It is considered only when the diagnosis is clear, the symptom pattern has been reviewed properly, and the likely benefit is meaningful.
DBS does not cure Parkinson’s disease or stop it from progressing. Its goal is to improve symptom control, reduce troublesome OFF time or dyskinesia in the right patient, and improve quality of life.
Careful movement disorder evaluation. Advanced treatment only when needed.
What Is Deep Brain Stimulation?
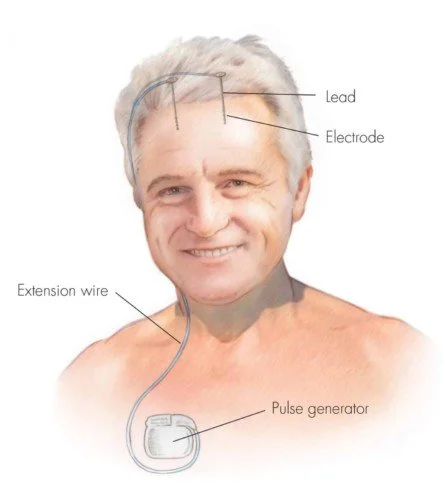
Deep Brain Stimulation, or DBS, is a treatment in which thin electrodes are placed in carefully selected areas of the brain and connected to a small pulse generator placed under the skin near the collarbone.
The system delivers controlled electrical stimulation to help regulate abnormal brain signals linked with certain movement symptoms.
For patients and families, the simplest way to understand DBS is this: it is an advanced treatment used to help control symptoms when medicines are no longer giving stable enough relief, or when medicine side effects have become too difficult.
DBS is not the right option for everyone. Proper patient selection, correct diagnosis, precise surgical planning, and expert follow-up are all important.


When DBS May Be Considered
DBS is usually considered when symptoms remain disabling despite thoughtful medical treatment.
In Parkinson’s disease, this often means the patient still shows meaningful benefit from medicines, but the benefit does not last well enough, OFF periods become troublesome, tremor remains difficult to control, or dyskinesia becomes a major problem.
In simple terms, DBS is not about doing surgery early because symptoms exist. It is about deciding whether advanced treatment may help when medicines are no longer giving the right balance of benefit, consistency, and quality of life.
This decision should always be based on careful movement disorder evaluation, not on fear, urgency, or guesswork.
Conditions DBS May Help
- Parkinson's disease
- Essential tremor
- Some forms of dystonia
- Movement-disorder symptoms that continue to cause major functional difficulty despite treatment
For Parkinson’s disease, DBS is mainly used to help motor symptoms such as tremor, stiffness, slowness, motor fluctuations, and dyskinesia in the right patient.
For essential tremor, it may help severe shaking that interferes with daily activities.
For dystonia, benefit depends on the type and cause, so evaluation must be individualized.
Not every tremor or every Parkinson’s diagnosis should lead to DBS discussion. The diagnosis must be correct first.
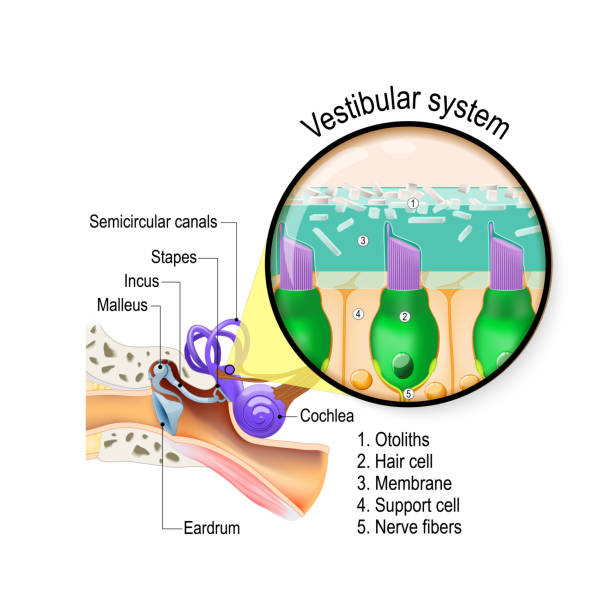
Who May Be a Suitable Candidate
- A clear diagnosis confirmed by a specialist
- Symptoms that interfere with daily life
- Shown meaningful benefit from Parkinson's medicines, but not reliable enough control
- Troublesome OFF periods, dyskinesia, or medication side effects
- Health that is reasonably suitable for surgery
- Realistic expectations about what DBS can and cannot do
- Family or caregiver support when needed
A patient may be less suitable if there is an unclear diagnosis, major memory or thinking problems, severe depression, hallucinations, marked balance issues as the dominant symptom, atypical Parkinsonism, or other medical issues that increase surgical risk.
This is exactly why detailed specialist evaluation matters so much.
How Patients Are Evaluated Before DBS
Before DBS is advised, the first question is not When can surgery be done? The first question is Is this the right patient, with the right diagnosis, at the right stage, for the right reason?
A proper DBS workup may include:
- Detailed neurological review
- Confirmation of diagnosis
- Assessment of symptom pattern and medication response
- Brain imaging such as MRI or CT
- Neurosurgical consultation
- Memory and thinking assessment
- Review of mood, balance, speech, swallowing, and general fitness for surgery
- Planning for support after the procedure
For Parkinson’s disease in particular, continued benefit from levodopa is often an important clue that DBS may help motor symptoms.
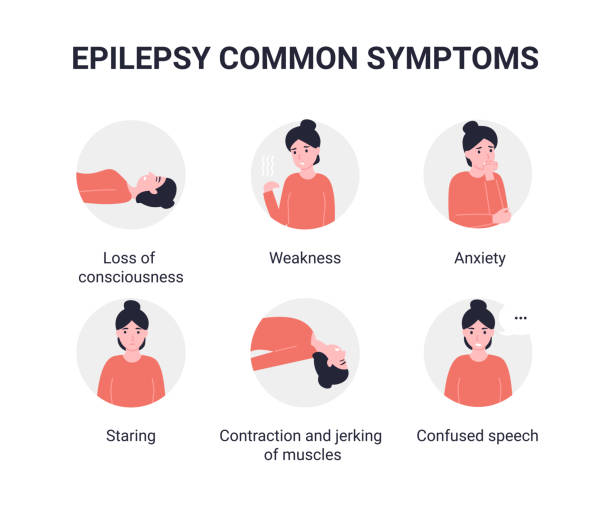
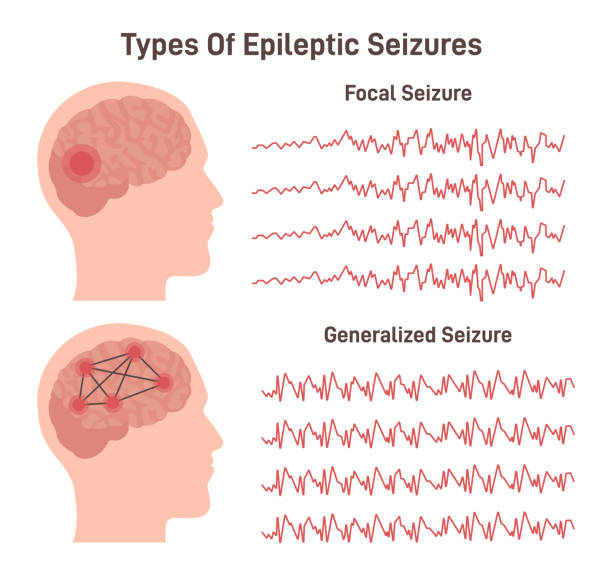
What the Procedure Involves
What tDBS usually involves placing one or more leads into carefully selected brain targets and connecting them to a pulse generator placed under the skin near the chest. Some details vary by surgical team and patient.
From a patient point of view, the important thing to know is this:
Careful planning happens first. Brain imaging and pre-surgical evaluation help the team plan safe and precise placement.
The leads are placed by the neurosurgical team.
The pulse generator is implanted under the skin, commonly below the collarbone.
Programming happens after recovery. Surgery is only one part of DBS. The system then needs expert adjustment over follow-up visits.
Patients often feel less anxious once they understand that DBS is not simply brain surgery and then done. It is a carefully managed treatment pathway with review and adjustment over time.
Benefits, Goals, and Limitations
For the right patient, DBS may help reduce tremor, stiffness, slowness, OFF periods, and dyskinesia. In some patients, it may also allow reduction of medication burden.
One of the main goals is to improve function and day-to-day quality of life.
But limits must be understood clearly.
DBS is not a cure. It does not stop Parkinson’s disease from progressing. It does not restore perfect health. And it does not improve every symptom equally.
Problems such as memory decline, swallowing difficulty, balance problems, or certain non-motor symptoms may not improve in the way patients hope.
That is why realistic expectations are so important. A good DBS discussion is not about hype. It is about matching likely benefit to the patient’s real symptom pattern and goals.

Risks and Important Considerations
DBS is generally considered safe in experienced hands, but it is still a serious procedure and should be approached with care.
Possible risks may include bleeding or stroke during surgery, infection, confusion after surgery, speech or balance issues, mood or thinking changes, hardware-related problems, and stimulation-related side effects.
Some side effects improve when settings are changed. This is one more reason programming follow-up is such an important part of the whole treatment process.
A balanced discussion of DBS should always include both sides: what it may help, and what it may not help. That honesty protects patients and leads to better decisions.
Life After DBS
Life after DBS involves follow-up, device programming, and medication review.
The stimulator is usually activated after recovery, and finding the right settings may take several visits over weeks or months. That gradual adjustment period is normal.
Patients should understand this clearly before surgery: the first programming visit is not the final result. Improvement often needs fine-tuning over time.
The device battery also needs long-term follow-up and may need replacement later, depending on the type of system and how it is used.
The best long-term results come when the patient, family, neurologist, and surgical team all understand that DBS is a continuing treatment process rather than a one-time eve

Dr. Siddharth Kharkar’s Approach to Advanced Treatment Decisions
Dr. Siddharth Kharkar’s approach is to recommend advanced treatment only when it is truly needed and when the clinical picture supports it.
For a patient with Parkinson’s disease, tremor, or another movement disorder, that means looking carefully at the exact diagnosis, how symptoms are affecting daily life, how well medicines are working, whether medicine side effects are becoming a major burden, and whether expectations from DBS are realistic.
DBS decisions should never be made in a rushed or overly commercial way. They should be made through careful diagnosis, specialist counseling, and thoughtful treatment planning.
The value of a specialist consultation is not only to discuss DBS. It is also to decide whether DBS is appropriate at all, whether other treatment changes should be tried first, and whether referral for advanced treatment workup makes sense at this stage.
Not every patient with Parkinson's disease or tremor needs DBS.
Not every patient with symptoms that are difficult to control needs surgery.
But when medicines are no longer giving stable relief, a specialist review can help clarify whether advanced treatment should be considered.
Frequently Asked Questions
What is DBS?
Is DBS a cure for Parkinson's disease?
Who may be considered for DBS?
Can DBS help tremor?
Can all Parkinson's patients have DBS?
What tests are needed before DBS?
What happens after surgery?
Are medicines always stopped after DBS?
What are the risks of DBS?