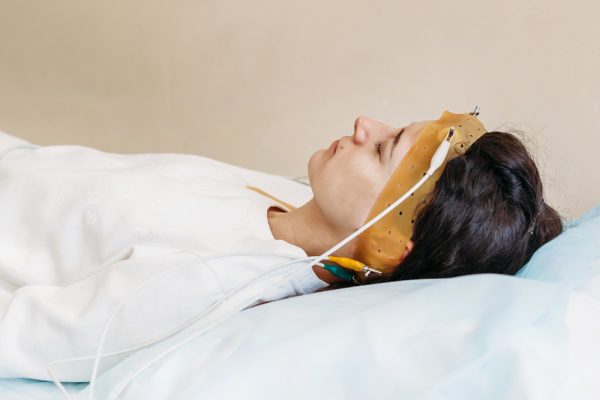
If you or a family member seems to shout, punch, kick, or act out vivid dreams during sleep, REM sleep behavior disorder may be one possible explanation. This condition deserves attention not only because it can lead to injury, but also because it can sometimes be linked with neurological disease.
Understanding the difference between an occasional restless night and a true sleep behavior disorder can help you take the right next step sooner. In many cases, a careful neurological assessment and a sleep study can bring much-needed clarity.
Medically guided by Dr. Siddharth Kharkar
Table of Contents
ToggleTrusted neurological guidance that turns complex symptoms into clear next steps. Focused on helping patients and families recognize REM sleep behavior disorder early, understand its neurological significance, and seek the right care without unnecessary fear or delay.
A Quick Answer
REM sleep behavior disorder is a condition in which a person physically acts out dreams during REM sleep, often with shouting, punching, kicking, or sudden movements. It matters because it can cause injury, disturb sleep, and in some cases be associated with neurological conditions that deserve specialist evaluation.
At a Glance
- REM sleep behavior disorder often causes dream enactment during sleep.
- Common signs include shouting, talking, punching, kicking, grabbing, or falling out of bed.
- People may remember vivid or frightening dreams if awakened.
- The condition can injure the person sleeping or their bed partner.
- Diagnosis usually requires clinical evaluation and an overnight sleep study.
- Treatment may involve safety changes, medication, and follow-up for associated neurological conditions.
What Is REM Sleep Behavior Disorder?
During normal REM sleep, the brain is active but the body’s muscles are largely kept still. This natural protection helps prevent us from acting out our dreams.
In REM sleep behavior disorder, that normal muscle quieting does not work as it should. As a result, the sleeping person may move, speak, or react physically to dream content.
This is why some people appear to be fighting, running, defending themselves, or shouting in their sleep. The behavior is usually not intentional, and many patients only learn about it after a bed partner or family member notices a pattern.
REM Sleep Behavior Disorder Symptoms to Watch For
Common Movements and Vocal Behaviors During Sleep
Symptoms can vary from mild to dramatic. Some people only have occasional limb movements or sleep talking, while others may have forceful movements that look purposeful.
Common REM sleep behavior disorder symptoms include:
- Talking, shouting, or screaming during sleep
- Punching, kicking, flailing, or grabbing
- Sudden jerking or jumping out of bed
- Acting out vivid, intense, or frightening dreams
- Remembering the dream clearly after waking
Many episodes happen in the second half of the night, when REM sleep becomes longer and more frequent.
When Symptoms Become Dangerous
This condition becomes especially concerning when the movements are forceful enough to cause injury. Patients may bruise themselves, strike a bed partner, hit furniture, or fall out of bed.
Even when the injuries are minor, repeated episodes can create anxiety around sleep for the whole household. That is often the point when families realize this is not simple restlessness.
How RBD Differs From Sleepwalking, Night Terrors, and Seizures
RBD is not the same as sleepwalking. Sleepwalking usually occurs in non-REM sleep, and the person is often confused when awakened.
Night terrors also behave differently. A person with RBD may often wake relatively alert and may recall the dream, while someone with a night terror is usually disoriented and does not clearly remember what happened.
Seizures can also sometimes be mistaken for abnormal sleep behaviors. That is one reason diagnosis should not rely on internet descriptions alone. A neurological review and sleep testing can help separate these possibilities.
Why REM Sleep Behavior Disorder Matters Neurologically
One of the most important things to understand is that REM sleep behavior disorder is not always just a sleep issue. In some patients, especially older adults with new onset symptoms, it can be associated with underlying neurological disease.
That does not mean every person with RBD will develop Parkinson’s disease or dementia. It does mean the condition should be evaluated thoughtfully rather than dismissed.
The Link With Parkinson’s Disease and Related Neurological Conditions
RBD has been associated with neurological conditions such as Parkinson’s disease, dementia with Lewy bodies, and multiple system atrophy. This association is one of the reasons neurologists take the condition seriously.
For some patients, RBD appears before more obvious neurological symptoms begin. In others, it occurs alongside an already recognized neurological diagnosis.
Why Early Neurological Evaluation Matters
An early evaluation gives you more than a label. It helps identify whether the problem is isolated, medication-related, linked to another sleep disorder, or part of a broader neurological picture.
It also creates a baseline. If future symptoms involving movement, balance, memory, or cognition appear, they can be recognized and monitored more effectively.
What Causes REM Sleep Behavior Disorder?
In simple terms, RBD happens when the normal protective loss of muscle activity during REM sleep is disrupted. The reasons for that disruption are not always the same.
Isolated RBD
Sometimes the condition appears on its own, without an immediately obvious cause. This is often called isolated or idiopathic RBD.
Although the patient may otherwise feel well, isolated RBD still deserves evaluation because of its known neurological associations.
RBD Linked to Neurological Disease
In some cases, RBD is associated with neurodegenerative conditions. This does not change the need to control symptoms and prevent injury, but it does influence long-term follow-up.
Medication-Related and Secondary Causes
Certain antidepressants and some other medical situations may trigger or worsen REM sleep behavior disorder. RBD can also be seen in association with narcolepsy and some other sleep or neurological conditions.
This is why medication review is part of good clinical care. A specialist looks not only at what the symptoms are, but also at what may be driving them.
How REM Sleep Behavior Disorder Is Diagnosed
Clinical History and Bed Partner Observations
The first step is often a detailed history. The description from a spouse, family member, or roommate can be extremely valuable because the person having the episodes may not fully realize what is happening.
Details such as dream recall, timing of episodes, injury, vocal behavior, and whether the person becomes alert quickly after waking all help guide the diagnosis.
Neurological Examination
A neurological examination helps assess for signs that may suggest an associated disorder. Depending on the situation, your doctor may look for tremor, stiffness, balance problems, memory concerns, or other neurological clues.
Sleep Study and REM Sleep Without Atonia
A formal overnight sleep study, usually video polysomnography, is often the most important test. It helps document abnormal behavior during REM sleep and identify the key physiological feature known as REM sleep without atonia.
The sleep study also helps rule out other problems, including obstructive sleep apnea or seizure-related events that may mimic RBD.
Treatment for REM Sleep Behavior Disorder
Making the Sleep Environment Safer
Safety comes first. If the episodes are active or forceful, the bedroom should be made safer right away.
This may include:
- Moving sharp or breakable objects away from the bed
- Padding nearby furniture
- Placing cushions or a mattress beside the bed
- Using protective bed barriers when appropriate
- Sleeping separately for a period if a bed partner is at risk of injury
These practical changes can reduce harm even before treatment is finalized.
Medications Such as Melatonin and Clonazepam
Medication is often used when symptoms are frequent, forceful, or dangerous. Melatonin is commonly considered because it may reduce symptoms and is often better tolerated.
Clonazepam is another well-known option and can be very helpful in selected patients. The right choice depends on age, fall risk, memory issues, sleep apnea, other medical conditions, and the patient’s overall neurological profile.
No medication should be started casually or copied from someone else’s prescription. Treatment needs to be individualized.
Treating Associated Conditions and Planning Follow-Up
If a medication is contributing to symptoms, that may need review. If another sleep or neurological disorder is present, treatment should address that as well.
Follow-up matters. In some patients, especially those with isolated RBD, periodic review may be advised to look for any evolving neurological symptoms over time.
When to See a Doctor for RBD Symptoms
You should seek medical attention if you or a loved one is regularly acting out dreams during sleep. The need is more urgent if there has been any injury, falling out of bed, striking a bed partner, or a noticeable worsening pattern.
You should also arrange an evaluation if these episodes are accompanied by tremor, slowed movement, stiffness, changes in balance, memory difficulties, or daytime neurological symptoms. Those details can be important.
In children and younger adults, unusual sleep behaviors also deserve assessment, especially when symptoms are frequent, severe, or associated with medications or narcolepsy.
Frequently Asked Questions About REM Sleep Behavior Disorder
Is REM sleep behavior disorder dangerous?
It can be. Some episodes are mild, but others can lead to bruises, cuts, falls, head injury, or injury to a bed partner.
Does REM sleep behavior disorder mean Parkinson’s disease is definitely coming?
No. It is associated with certain neurological disorders, but it is not a guarantee that a person will develop one. The right approach is careful evaluation and appropriate follow-up, not panic.
Can antidepressants trigger REM sleep behavior disorder?
Yes, in some patients antidepressants may trigger or worsen RBD-like symptoms. This should be reviewed by a doctor rather than handled by stopping medication abruptly on your own.
How is REM sleep behavior disorder confirmed?
Yes, in some patients antidepressants may trigger or worsen RBD-like symptoms. This should be reviewed by a doctor rather than handled by stopping medication abruptly on your own.
Can REM sleep behavior disorder be treated?
Yes. Treatment often improves safety and symptom control. Management may include bedroom safety measures, medication, and follow-up for associated sleep or neurological conditions.
Is this the same as a seizure disorder?
Not necessarily. Some sleep-related seizures can resemble abnormal nighttime behavior, which is why proper assessment is important.
Get the Right Neurological Guidance for Troubling Sleep Behaviors
If you or someone close to you is shouting, kicking, punching, or acting out dreams during sleep, it is worth getting a proper neurological and sleep evaluation. A clear diagnosis can reduce uncertainty, improve safety, and help identify whether there is a broader neurological issue that needs attention.
A careful consultation can help answer the questions that matter most: Is this really REM sleep behavior disorder, what is causing it, how can injuries be prevented, and what should be monitored going forward?
Troubling sleep behaviors should not be ignored, especially when they are repetitive, forceful, or linked with injury. Book a neurological evaluation with Dr. Siddharth Kharkar to understand the symptoms clearly, confirm the diagnosis properly, and create a treatment plan that is both practical and medically sound.