Some people with myasthenia gravis do not notice the condition all at once. The earliest changes may seem small, inconsistent, or easy to dismiss, such as one eyelid drooping by evening, double vision that comes and goes, speech becoming unclear after talking for a while, or chewing becoming difficult before a meal is finished.
Because these symptoms can look like eye strain, stress, fatigue, or simply “getting tired,” diagnosis is sometimes delayed. The good news is that myasthenia gravis is treatable, and recognizing the early pattern can help you get the right evaluation sooner.
If you or a family member have unexplained droopy eyelids, double vision, swallowing difficulty, speech changes, or weakness that gets worse with repeated activity, a neurological assessment is worth considering.
Medically guided by Dr. Siddharth Kharkar
Trusted neurological guidance that turns complex symptoms into clear next steps. Focused on helping patients and families recognize myasthenia gravis warning signs early so they can seek the right care without delay.
Quick answer: What are the early symptoms of myasthenia gravis?
Table of Contents
ToggleMyasthenia gravis early symptoms often begin with weakness in muscles that are used repeatedly through the day. The most common early signs include droopy eyelids, double vision, difficulty chewing, swallowing changes, a soft or nasal voice, neck weakness, and arm or leg weakness that feels worse after activity and better after rest. In some people, symptoms stay limited to the eyes at first. In others, they gradually involve speaking, swallowing, breathing, or limb movement.
Myasthenia gravis at a glance
- It is a condition in which communication between nerves and muscles becomes impaired.
- Symptoms often fluctuate instead of staying constant.
- Eye symptoms are a common early starting point.
- Speech, swallowing, chewing, neck, arm, or leg weakness may appear later or sometimes early.
- Breathing difficulty or worsening swallowing trouble needs urgent medical attention.
- Diagnosis may involve a neurological examination, antibody blood tests, EMG, and sometimes chest imaging.
- Treatment can improve symptoms and function significantly in many patients.
Why early myasthenia gravis symptoms are often missed
Symptoms can come and go
One reason myasthenia gravis is missed early is that the symptoms are not always present at the same intensity. A person may wake up feeling relatively normal, then notice their eyelids drooping later in the day. Someone else may speak clearly at the start of a conversation, but their words become slurred or nasal after prolonged talking.
This fluctuating pattern can confuse both patients and families. Many people assume a serious neurological condition would cause constant weakness, but myasthenia gravis often behaves differently.
The first signs may look like eye strain, fatigue or stress
Early MG symptoms are easy to misread. Double vision may be blamed on poor sleep or screen time. Difficulty chewing may be dismissed as a dental issue. Trouble holding the head up by evening may be written off as posture, muscle strain, or exhaustion.
Because these signs do not always appear together at first, people may focus on each symptom separately instead of recognizing the larger pattern.
Weakness often worsens with repeated use and improves with rest
This is one of the most important clues. In myasthenia gravis, weakness commonly becomes more noticeable when a muscle is used repeatedly. The eyelids may droop more after reading. Speech may become less clear after a long conversation. Chewing may become difficult halfway through a meal. A short period of rest may improve the symptom, at least temporarily.
That “worse with use, better with rest” pattern is not something patients should ignore.
Early symptoms patients often miss
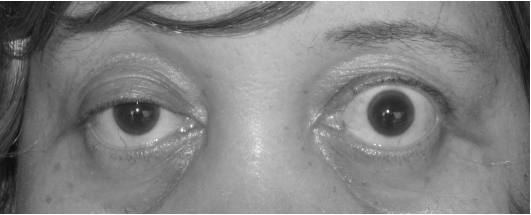
Droopy eyelids and double vision
For many people, the earliest signs involve the eyes. One or both eyelids may start to droop, especially later in the day. Some people notice they are lifting their eyebrows more often, tilting their head back to see more clearly, or closing one eye to read.
Double vision is another classic early symptom. It may happen only when looking in certain directions, only in the evening, or only after the eyes have been used for a while. Because it can be intermittent, people sometimes delay evaluation.
If droopy eyelids or double vision keep returning, especially when tired, it is important to think beyond routine eye strain. Ocular myasthenia gravis can begin with eye symptoms alone, but in some patients the condition later affects other muscle groups.
Trouble chewing, swallowing or speaking clearly
Myasthenia gravis can affect the muscles of the face, jaw, mouth, and throat. In early stages, this may show up in small ways. A person may feel that chewing becomes tiring before the meal is over. They may avoid tougher foods because the jaw seems to “give up” too quickly.
Speech changes can also be subtle at first. The voice may become soft, nasal, husky, or slightly slurred after talking for some time. Swallowing problems may begin as occasional coughing while drinking water, repeated throat clearing, or a sense that food is not moving down normally.
These are especially important symptoms because they affect nutrition, safety, and quality of life. They also deserve prompt attention if they are getting worse.
Weakness in the neck, shoulders, arms or legs
Not all early MG symptoms are dramatic. Sometimes the first complaint is that holding the head upright feels unusually tiring by the end of the day. Some people notice difficulty lifting the arms to wash their hair, brush their teeth, or reach overhead. Others feel more weakness climbing stairs or getting up from a seated position.
This is not the same as ordinary tiredness after a long day. The weakness may feel oddly selective, fluctuate from day to day, and become more noticeable with repeated effort.
Shortness of breath or unusual fatigue with activity
Breathing-related symptoms should never be taken lightly. Early breathing involvement may feel like unusual breathlessness during activities that were previously easy, trouble taking a deep breath, or increased shortness of breath when lying flat.
Some patients describe it not as “I am breathless all the time,” but as “my breathing muscles seem to tire.” That distinction matters. Even mild breathing symptoms deserve serious attention in someone with possible MG.
When symptoms stay around the eyes and when they spread
In some people, symptoms remain limited to the eyes for a prolonged period. In others, the condition spreads over time to involve speaking, swallowing, the neck, limbs, or breathing muscles.
That is why recurring eye symptoms should not be dismissed just because the rest of the body seems unaffected at the beginning. A careful evaluation can help determine whether the weakness is confined to the eye muscles or part of a broader neuromuscular problem.
When myasthenia gravis symptoms become urgent
Trouble swallowing or repeated choking
If swallowing becomes clearly difficult, if food or liquids are repeatedly “going the wrong way,” or if there is frequent choking or coughing during meals, this should be treated as more than a minor symptom. Delayed evaluation increases the risk of aspiration and related complications.
Breathing difficulty or rapidly worsening weakness
Breathing problems, chest tightness from muscle fatigue, rapidly worsening weakness, or difficulty holding up the head can become urgent. If there is significant shortness of breath, worsening swallowing, or clear breathing distress, seek emergency medical care immediately.
It is always better to act early than to wait and hope severe symptoms settle on their own.
How myasthenia gravis is diagnosed
Medical history and neurological examination
Diagnosis begins with pattern recognition. A neurologist will ask when the symptoms occur, whether they fluctuate, which muscle groups are involved, and whether rest improves the weakness. A focused neurological examination can reveal clues that point toward a neuromuscular junction problem.
Antibody blood tests
Many patients with myasthenia gravis have abnormal antibodies that interfere with communication between nerves and muscles. Blood tests may look for antibodies such as acetylcholine receptor antibodies and, in some cases, other related antibodies depending on the clinical picture.
A positive antibody test can strongly support the diagnosis, but the condition is not ruled out simply because one test is negative. The full clinical picture still matters.
EMG and repetitive nerve stimulation
Electrodiagnostic testing can be very helpful. EMG and repetitive nerve stimulation are used to look for the characteristic communication problem between nerves and muscles. In selected cases, a more specialized single-fiber EMG may be recommended.
These tests are useful because they move the evaluation from “something feels wrong” to objective evidence of how the nerve-muscle connection is functioning.
Imaging of the thymus when needed
The thymus gland can be relevant in myasthenia gravis, so chest imaging may be done in some patients to look for thymic enlargement or a thymoma. This is not the first thing every patient notices, but it is an important part of a complete diagnostic workup when MG is suspected.
Treatment for myasthenia gravis and what to expect
Medicines that improve nerve-muscle communication
Some medications help improve communication between the nerves and muscles, making it easier for the muscles to work. These can reduce symptoms and help patients function better through the day.
Immune treatments and longer-term control
Because myasthenia gravis is an immune-mediated condition, treatment may also include medicines that calm the abnormal immune response. The exact approach depends on symptom severity, which muscles are involved, how quickly symptoms are progressing, and the patient’s overall health.
When surgery may be considered
In some patients, especially when the thymus is involved or when the clinical situation fits established treatment pathways, surgery may be part of care. This decision is individualized and should be discussed carefully with a neurologist and the treating team.
Why early diagnosis can improve day-to-day function
The biggest practical benefit of early diagnosis is not only disease labeling. It is better function, safer swallowing and breathing, more confident daily activity, and a more timely treatment plan.
Many patients feel relieved simply because the pattern finally makes sense. Once the correct diagnosis is made, treatment decisions become clearer and quality of life often improves.
When to see a neurologist
You should consider a neurological evaluation if you have any of the following:
- droopy eyelids that keep returning
- double vision that comes and goes
- speech that becomes slurred, soft, or nasal after talking
- chewing fatigue during meals
- swallowing difficulty, repeated coughing, or choking
- weakness in the neck, arms, or legs that worsens with repeated use
- unexplained shortness of breath linked to weakness or fatigue
A pattern like this deserves proper assessment, especially when symptoms fluctuate rather than remain steady.
Frequently asked questions
Can myasthenia gravis start only with eye symptoms?
Yes. Some patients begin with droopy eyelids or double vision alone. This is often referred to as ocular myasthenia gravis. Even when symptoms begin only in the eyes, they should still be evaluated carefully.
Can myasthenia gravis be mistaken for another condition?
Yes. It may initially be confused with eye strain, fatigue, stress, age-related weakness, thyroid eye disease, stroke-related concerns, or other neurological and muscular conditions. That is one reason diagnosis may be delayed.
Do symptoms of myasthenia gravis come and go?
Can myasthenia gravis be mistaken for another condition?
Yes. It may initially be confused with eye strain, fatigue, stress, age-related weakness, thyroid eye disease, stroke-related concerns, or other neurological and muscular conditions. That is one reason diagnosis may be delayed.
Is myasthenia gravis treatable?
Yes. While it is a chronic condition, there are effective treatments that can improve symptoms and daily function. The right treatment plan depends on the individual patient and the pattern of disease involvement.
When is myasthenia gravis an emergency?
It becomes urgent when swallowing is getting worse, choking is recurrent, breathing becomes difficult, or weakness progresses quickly. In those situations, immediate medical attention is important.
Take the next step
If you have symptoms that suggest myasthenia gravis early symptoms are being overlooked, do not ignore the pattern simply because the weakness comes and goes. Fluctuating droopy eyelids, double vision, swallowing difficulty, speech change, or weakness that worsens with use deserves a closer look.
A timely neurological evaluation can clarify what is happening and help you move toward the right treatment plan with confidence.