![Epilepsy surgery in India – Where, why and costs 1 Epilepsy Surgery Cost In India 2023 [Best Epilepsy Treatment In India]](https://drkharkar.com/wp-content/uploads/2025/05/Simple-evaluation-for-Epilepsy-surgery-in-India-1024x896.webp)
1. Why is Epilepsy surgery in India done?
Some people have seizures. These happen because of uncontrolled electricity in the brain.
This condition is called “Epilepsy”.
About 80% patients stop having seizures when they take medications.
But 20% people keep having seizures despite taking 2 or more medications. These patients have “Medically resistant epilepsy”.
They need Epilepsy surgery to stop their seizures.
2. Is Epilepsy surgery done in India?
Yes. All types of epilepsy surgeries can be done in India.
In the USA epilepsy surgery is very common. Larger hospitals (like UCSF, where I was educated) do about 2-3 epilepsy surgeries per week.

In India, Epilepsy surgery is less common. This is because:
– Patients & doctors are not aware of it.
– Fewer doctors are trained in Epilepsy surgery.
– Cost
– Fear of complications
– But most importantly, many Indians have a sad, hopeless and completely wrong belief that epilepsy is uncontrollable.
3. What are the types of Epilepsy Surgery?
There are many types of Epilepsy surgery.
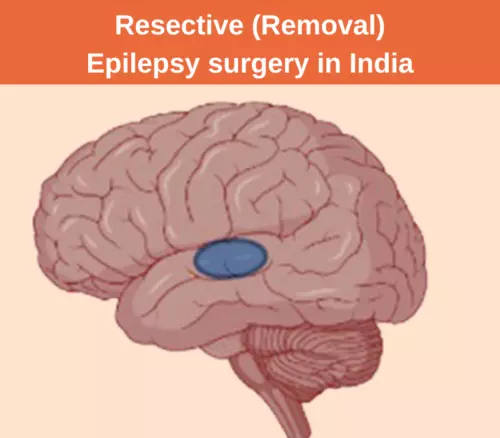
RESECTIVE (REMOVAL SURGERY):
This is the best Epilepsy surgery.
The bad seizure-producing part of the brain is removed. This stops seizures.
VAGUS NERVE STIMULATION (VNS):
In some cases, resective (removal) surgery is difficult. This can happen if the bad part is too large, or is near important brain parts.
In such cases, Vagus Nerve Stimulation (VNS) surgery is done. This is a faster surgery.
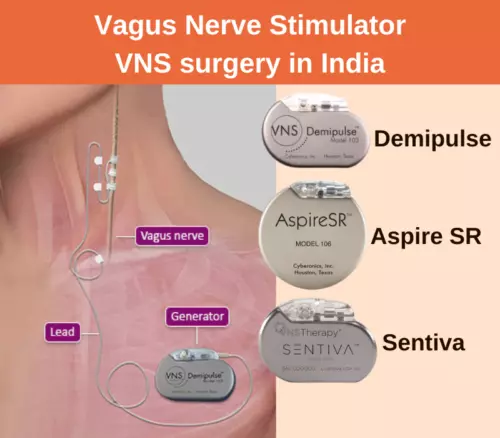
A small battery is placed in the skin over the chest. A thin wire is attached to a nerve below the neck skin.
The VNS device sends small currents to the brain which prevent seizures.
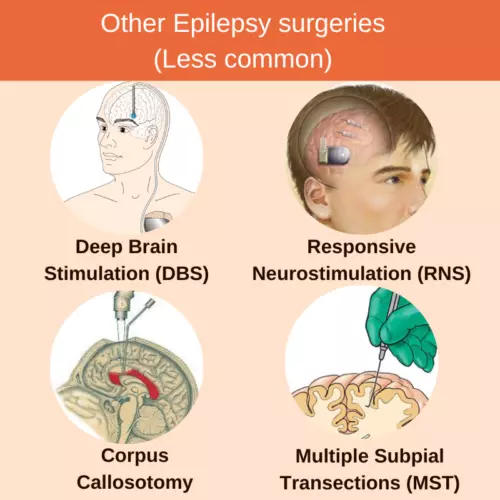
OTHER SURGERIES:
Other surgeries are done in special situations. For example, corpus callostomy can be done instead of VNS if the patient cannot afford VNS.
4. What tests Need to be done before Epilepsy surgery?
The routine tests done before every epilepsy surgery are listed below.
![Epilepsy surgery in India – Where, why and costs 1 Epilepsy Surgery Cost In India 2023 [Best Epilepsy Treatment In India]](https://drkharkar.com/wp-content/uploads/2025/05/Simple-evaluation-for-Epilepsy-surgery-in-India-1024x896.webp)
We try to answer many questions with these tests:
In some patients, we need to do additional tests to answer these questions. In most patients, these tests are not needed.
In very rare cases, the location of the bad part is unclear even after these tests. In such cases, we need to record EEG directly from the brain.
This is done by placing thin stiff wires in the brain. This process is called stereo-EEG.
5. What is Video EEG Monitoring (Epilepsy Monitoring)?
The patient is admitted for continuous EEG monitoring. During this time, we may reduce medications so that the patient has seizures.

We try to capture at least 2 seizures of each type.
For example, if the patient has one seizure type where he falls down, and another type where he starts smacking his lips, then we capture 2+2 = 4 seizures.
If you have seizures frequently, epilepsy monitoring may take just 1-2 days. In other people, it may take 7 days or more.
6. What is the success rate of Epilepsy surgery in India?
The success rate of epilepsy surgery is high but not 100%.
The success rate depends on the type of epilepsy, and the type of epilepsy surgery.
For example:
· The success rate of Resective surgery can be more than 80%.
· The success rates of other surgeries are lower, but usually quite good.

· After VNS, most patients seizures decrease by 50% or more. Specifically, drop attacks, where patients fall and hurt themselves, are significantly reduced.
The success rate will be discussed with you after the presurgical tests.
7. Will my medications stop after Epilepsy surgery?
The goal of epilepsy surgery is to stop your seizures.
Approximately 50% patients are able to stop their medications after Epilepsy surgery.
However, other patients need to keep taking their medications. Some patients may be able to reduce their medications.
8. What are the possible complications?
Any surgery has some risks of anaesthesia and infection.
In resective surgery, there is a concern that surrounding areas may be damaged. This depends on the exact location of the bad part.
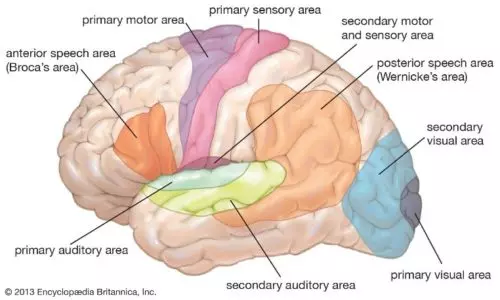
Surgery needs to be done very carefully if the bad part is close to important brain areas (e.g., speech & memory areas).
Thankfully, stopping seizures after resection improves thinking and memory in many people. This is because the healthy parts of the brain work better.
All possible complications will be discussed with you after the presurgical tests.
9. What is the cost of Epilepsy surgery?
Patients need different evaluations and surgeries, so the cost is different for each patient.
For example:
If our patient has frequent seizures and requires a simple resection, the total cost is between 4.5 – 5 lakhs. This is the total cost, including all tests.
| Test | Cost in India |
|---|---|
| STEP 1: EVALUATION | |
| MRI | Rs. 12,000 |
| PET & MRI-PET fusion | Rs. 15,000 |
| functional MRI (fMRI) | Rs. 12,000 |
| Video-EEG monitoring (3 days) | Rs. 30,000 x 3 = Rs. 90,000 |
| Psychiatry & Neuropsychological testing | Rs. 6,000 |
| Total cost of evaluation | Rs. 1.35 Lakh |
| STEP 2: SURGERY ITSELF | |
| Resective surgery with intraoperative Electrocorticography | Rs. 3.5 Lakh |
| TOTAL COST | Rs. 4.95 Lakh |
VNS surgery is very expensive. The major part of the expense is the device, which has to be imported.
| Test | Cost in India |
|---|---|
| VNS procedure cost (cost of placement) | Rs. 1.5 Lakh |
| VNS device cost – Demipulse | Rs. 8.5 Lakh |
| VNS device cost – Aspire SR | Rs. 10.5 Lakh |
| VNS device cost – Sentiva (newest model) | Rs. 14.5 Lakh |
10. Should I (or my child) have Epilepsy surgery?
If a person has medically resistant epilepsy, I usually encourage them to have epilepsy surgery, if:
The patient really has medically resistant epilepsy.
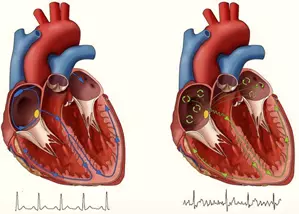
1. Patients may be misdiagnosed. For example, people with heart rhythm issues or stress-related seizures may be wrongly diagnosed with epilepsy.
2. Sometimes, the type of medication or the dose may be incorrect for the type of epilepsy.
3. Sometimes, patients have seizures because they don’t take their medications.
Possible complications are acceptable to the patient.
For example, if someone’s right hand remains very strong but fine motor skills change after surgery, it could significantly affect a painter.

But, if the patient is a manual labourer, it may not matter much.
The patient should understand there is no 100% guarantee. No surgery has a 100% guarantee.
11. What if I decide to continue just with medications?
There is a chance that new epilepsy medications may be discovered in the future. But it is worth understanding the history of medication resistant epilepsy.

In 2000, Dr. Kwan and Dr. Brodie conducted an important study. They discovered that if two seizure medications didn’t work, the chances of becoming seizure-free with medications alone was less than 5%.
In the 20+ years since that study, many new seizure medications have been invented. These have fewer side-effects but unfortunately, their efficacy is not very different (see below).
The number of patients who don’t respond to medications remained nearly the same.
12. What about the newest medications?
I was hopeful about a new medication called Perampanel because it acts in a completely different way as compared to other anti-seizure medications.
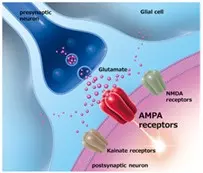
Unfortunately, me and other neurologists have found that it is not very effective in most people with medically resistant epilepsy.
Many of the other “newer” medications like Eslicarbazepine are the same as the older medications (carabamazepine) with only minor differences.
For example, Eslicarbazepine can be taken once daily, whereas carbamazepine needs to be taken twice daily.
13. What are the possible complications of waiting?
I, too, hope for much more effective medications in the future. But our need for treatment is in the present.

Waiting has drawbacks.
1. If seizure surgery can make a person seizure free, waiting means wasting productive years of his/her life.
2. Brain damage is a worry, for patients who have frequent seizures. Waiting in such cases may cause permanent thinking and memory problems.
3. If patients have many seizures, other parts of the brain may also become abnormal and start producing seizures.
14. Can almost all patients with Epilepsy have a full, normal life?
Yes.
Caution: This information is not a substitute for professional care. Do not change your medications/treatment without your doctor’s permission.
