
What exactly is Epilepsy?
Table of Contents
ToggleTo know the exact meaning of Epilepsy, you need to understand what is a seizure.
You can read all about seizures here.
In summary, a seizure is a temporary electrical storm in the brain. It is caused by unregulated spikes of electricity.
Now:
If a person keeps having seizures repeatedly, he/she can be said to have a TENDENCY to have seizures. This TENDENCY to have repeated seizures is called EPILEPSY.
What are provoked seizures?
Any person’s brain can have a seizure if the provoking stimulus is very strong.
So, a person can have seizures, even if there is no underlying tendency to have seizures (Epilepsy).
- People who consume cocaine may get seizures. This may happen even though their brain does not have a tendency to have seizures (Epilepsy).
- People who abuse alcohol and then suddenly stop it may get seizures. This may happen even if their brain does not have a tendency to have seizures (Epilepsy).
These seizures are called provoked seizures. There is a strong agent that provoked the brain into having a seizure.
Would you say that a person who abuses cocaine has Epilepsy? Most of the time, the answer is no. There is no underlying tendency to have seizures, it is purely the cocaine which is at fault.
So, provoked seizures (even if they happen repeatedly) usually do not indicate Epilepsy.
Could you provide some examples?
Sure!
John & Max:
Let’s consider two people:
- John had a seizure after he received an Antibiotic called Imipenem – which is known to cause seizures in some people.
- Max, a 12-pack a day alcoholic, had a seizure after he suddenly stopped drinking alcohol.
Does John or Max have Epilepsy?
No! Because both of them had seizures that happened after strong provocation.
Sid:
Let’s consider another person:
- Sid sleeps only for 6 hours on consecutive nights trying to get something done. On the third morning, he has multiple jerks of his upper body, followed by a generalized seizure.
- He neglects this, and the next week, the same thing happens again.
Was there a strong provocation?
No, the sleep deprivation was mild.
Does Sid’s brain have a tendency to have recurrent seizures?
Yes, based on the fact that he had seizures on two successive weeks.
Sanjay:
- Sanjay had one unprovoked seizure when he was 3 years old.
- He has had no seizures since then, and is now 55 years old.
Does Sanjay’s brain ever have an increased tendency to have seizures?
Probably not, considering that he had only one seizure and then none in the last 52 years.
Pooja:
- Pooja had 15 seizures between 5 and 10 years of age.
- Since that time she never had a seizure, and is now 60 years old.
Did Pooja’s brain ever have an increased tendency to have unprovoked seizures?
Yes, between 5-10 years of age, she certainly had many seizures. So she had Epilepsy.
Does Pooja’s brain still have an increased tendency to have unprovoked seizures?
Probably not, considering she has had no seizures for the past 50 years!
Therefore, it is certainly possible to outgrow your Epilepsy.
Is the history of a person always sufficient for making a diagnosis of “Epilepsy”?
If we have a long enough history, probably yes.
But – and this is a very common occurrence – let’s say a 5th person: Prasad – has a single seizure and rushes to your clinic. How can you predict whether he will have more seizures?
In addition to the history, two tests help in estimating the chance that a person will have recurrent seizures: An MRI and an EEG. An abnormal result in any of these tests indicates a higher tendency to have seizures. These tests are described in more detail here:
Is Epilepsy Common?
Yes!
About 1% of the general population has Epilepsy.
An easier way to think of it is: If there are 200 people in any sort of group, e.g. a social gathering, then 1-2 people there will have Epilepsy.
What are the types of Epilepsy?
There are two basic types of Epilepsy:
- Focal Epilepsy
- Primary Generalized Epilepsy
These types are based on the patient’s type of seizures.
It is simple to understand these two types, if you have read the seizure article.
Some patients have both kinds of Epilepsy. In other patients, doctors are unable to make up their mind about the kind of Epilepsy the patient has.
So, the International League against Epilepsy (ILAE) has defined 4 different groups of Epilepsy.
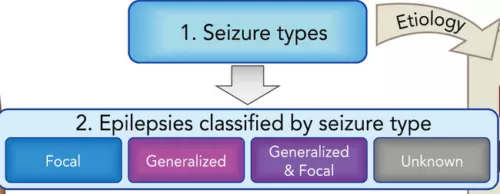
https://www.researchgate.net/figure/Framework-for-epilepsy-classification-The-etiological-framework-can-also-be-used-for_fig1_304375138
So, what are “Epilepsy Syndromes”?
The ILAE defines an “Epilepsy Syndrome” as follows:
| Epilepsy Syndrome |
|---|
“An epilepsy syndrome refers to a cluster of features incorporating seizure types, EEG, and imaging features that tend to occur together.” |
People with Epilepsy in the same “Group” share many characteristics. They may all be of the same age, have the same seizure types
Allow me explain it simply:
Around the 1950s, doctors from France realized that patients with Epilepsy tended to fall into “Groups”. They started to see patterns of age, gender, response to medications etc… Because it helped them to focus their thinking, they labelled these groups with different names.
As this practice picked up steam, more and more such groups were defined by other doctors.
Therefore, the list of Epilepsy Syndromes is ever expanding. Every once in a while, one more doctor detects a new group of people who share similar characteristics – a new Epilepsy Syndrome.
For example:
| An example of patients sharing similar characteristics |
|---|
A certain group could be just children who have short episodes of blanking out during the day. They never have big shaking seizures (Generalized tonic-clonic seizures). Before the children turn 15, the seizures usually stop by themselves. |
We now call this Epilepsy syndrome “Childhood Absence Epilepsy” (CAE). These children are said to have “Childhood Absence Epilepsy”.
Such groupings of people (Epilepsy syndromes) are much more common in children and young adults.
In older patients, the most common Epilepsy is that starting from one area of the brain (Focal Epilepsy). In other words, Epilepsy in adults looks all the same. There is not enough grouping (clustering) of characteristics to divide adults with Epilepsy into separate syndromes.
What are a few examples of “Epilepsy Syndromes”?
Here are a few examples of Epilepsy syndromes.
Please note:
- These are more common in children & young adults
- Their names give you many clues about their characteristics
| Epilepsy Syndrome | Common things |
|---|---|
| Childhood Absence Epilepsy (CAE) | All patients are children. They have blank staring episodes which last for a few seconds to a few minutes. These are described as “day dreaming” or being “Absent-minded” by their teachers. The poor children may be accused of not paying enough attention in class. The EEG is very characteristic – a particular pattern called “3Hz spike-and-wave” is seen in all patients. |
| Juvenile Myoclonic Epilepsy (JME) | As the first word indicates, this epilepsy syndrome starts in Juveniles (12 to 18 years of age). The word “Myoclonus” means “sudden jerks”. These patients get sudden jerks of the upper body, especially when they are sleep deprived. They may also have very violent generalized convulsions. The EEG is again very characteristic – a particular pattern called “polyspike-and-wave” is seen in all patients. |
Focal Epilepsy
|
These patients don’t share many common characteristics. Focal Epilepsy can happen at any age. These patients have “Focal Seizures”, that is – seizures that begin in one part of the brain. Focal Epilepsy can be due to many, many different reasons such as brain tumors, or blood vessel knots, or developmental problems called “Focal Cortical Dysplasias”. |
Complete list of Epilepsy Syndromes
Many other Epilepsy Syndromes have been described.
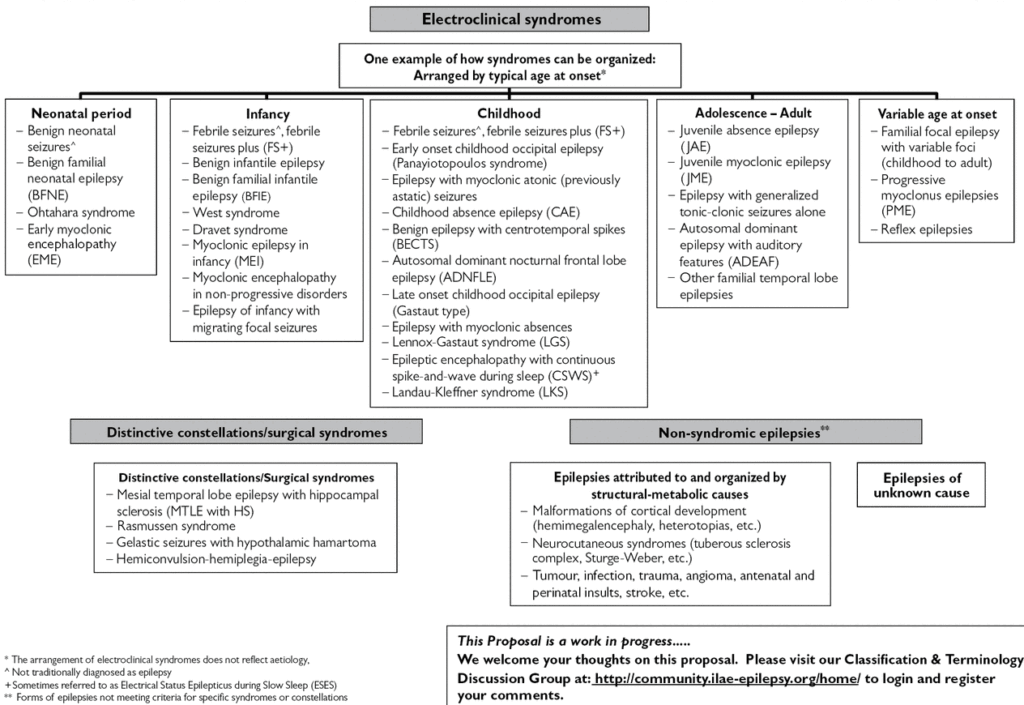
Here is a comprehensive diagram from 2010. It is not essential to remember every Epilepsy syndrome. If you have one of these, your doctor will discuss it with you.
Below the diagram, you will find a text list. It is difficult for me to write in detail about each syndrome.
But I will try my best. The Epilepsy Syndromes I have written about will be marked in blue in the list below:
Nenonate (First 4 weeks)
- Benign neonatal seizures
- Benign familial neonatal epilepsy (BFNE)
- Ohtahara syndrome
- Early Myoclonic encephalopathy (EME)
Infancy (in the first year of life)
- Febrile seizures , Febrile seizures plus (FS+)
- Benign infantile epilepsy
- Benign familial infantile epilepsy (BFIE)
- West syndrome
- Dravet syndrome
- Myoclonic epilepsy in infancy (MEI)
- Myoclonic encephalopathy in non-progressive disorders
- Epilepsy of infancy with migrating focal seizures
Childhood
- Febrile seizures , Febrile seizures plus (FS+)
- Early onset childhood occipital epilepsy (Panayiotopoulos syndrome)
- Epilepsy with myoclonic atonic (previously astatic) seizures
- Childhood absence epilepsy (CAE)
- Benign epilepsy with centrotemporal spikes (BECTS)
- Autosomal dominant nocturnal frontal lobe epilepsy (ADNFLE)
- Late onset childhood occipital epilepsy (Gastaut type)
- Epilepsy with myoclonic absences
- Lennox-Gastaut syndrome (LGS)
- Epileptic encephalopathy with continuous spike-and-wave during sleep (CSWS)+
- Landau-Kleffner syndrome (LKS)
Adolescence – Adult
- Juvenile absence epilepsy (JAE)
- Juvenile myoclonic epilepsy (JME)
- Epilepsy with generalized Tonic
- clonic seizures alone
- Autosomal dominant epilepsy with auditory features (ADEAF)
- Other familial temporal lobe epilepsies
Variable age at onset
- Familial focal epilepsy with variable foci (childhood to adult)
- Progressive myoclonus epilepsies (PME)
- Reflex epilepsies
Distinctive Constellations/Surgical syndromes
- Mesial temporal lobe epilepsy with hippocampal sclerosis (MTLE with HS)
- Rasmussen syndrome
- Gelastic seizures with hypothalamic hamartoma
- Hemiconvulsion-hemiplegia-epilepsy
Epilepsies organized by structural/metabolic causes
- Malformations of cortical development (hemimegalencephaly, heterotopias, etc.)
- Neurocutaneous syndromes (tuberous sclerosis complex, Sturge-Weber, etc.)
- Tumor, infection, trauma, angioma, antenatal and perinatal insults, stroke, etc
| Caution: This information is not a substitute for professional care. Do not change your medications/treatment without your doctor’s permission. |
